
Clinical and Epidemiological Characteristics of Orbital Floor Fractures, Rebuilt with Titanium Mesh
*Corresponding Author(s):
Giselle JRADepartment Of Dental Surgen, National Medical Center Century XXI, Mexico
Tel:+52 5556276900,
Email:giselle_juarez@hotmail.com
Abstract
Orbital fractures are an important public health problem. The evaluation of this study was focused on patients with orbital floor fractures, showing the risk involved in anatomical structures, as well as the importance of clinical-tomographic correlation to determine the diagnosis. Precise and better adaptation of the implant to rebuild the floor of the eye socket. A descriptive, retrospective, cross-sectional study of the clinical-epidemiological characteristics of patients with orbital floor fractures treated surgically by titanium mesh reconstruction was carried out in Maxillofacial Surgery at the XXI Century National Medical Center. In the period from 2013-2018. The results were 159 patients with orbital fractures, of whom 157 were surgically managed: 157 with titanium mesh reconstruction and 2 surgical explorations without implants. The mean age 39.35 years (max: 86 min: 18), prevailing in males: 84.27%, 70 cases with orbital floor fracture, 69 orbital floor and medial wall fracture, 20 orbital floor fracture with another facial fracture, and 1% in panfacial fractures. 84% were secondary to physical aggression and 16% accidents of which 11% were by motorcycle, bicycle or falls and 5% by vehicle, 97% with periorbital edema, 40% with limited eye movements, 30% ecchymosis, 29% hyposphagma,18% emphysema, diplopia in 88%, 1.25% presented amaurosis.
Keywords
Fracture; Mesh; Orbit; Reconstruction; Titanium
INTRODUCTION
Orbital floor fractures are part of facial third thirds fractures, a public health problem when associated with car accidents and violence, they represent 0.3% of the total body surface [1-3]. Orbital trauma involves demographic, ethnic, socioeconomic issues, among others. Most orbital fractures are the result of forceful forces. Producing when an object larger than the size of the orbit hits the eye, the impact energy is transmitted through the orbit, causing fracture of the orbital floor and / or medial wall (thinner surfaces), which can cause displacement of the eyeball, although it does not usually cause its outbreak. The frequency of orbital floor fractures depends on various factors and conditions: sociodemographic, socioeconomic, and biomechanical. Direct orbital floor fractures may be single or extend to other walls and / or involve the orbital rim [4].
BACKGROUND
MacKenzie in Paris first describes orbital floor fractures in 1844. In 1957, Smith and Regan mention entrapment of the inferior rectus muscle with decreased eye motility in orbital floor fractures, and the term "burst fracture" was first used [5]. Two theories associated with the kinematics of orbital floor fractures are highlighted in the literature: hidrául hydraulic theory (fracture of the orbital floor by sudden increase in hydraulic pressure, with direct compression on its weakest surface: medial wall and orbital floor). The second (less approved): Fracture occurs when a large object hits the orbital rim, dispersing energy without displacement of the orbital content. If the intraorbital pressure is higher, the orbital content can be forced and herniated projecting into the maxillary sinus. Larry H Hollier reports 12 reconstructed patients with 0.25mm resorbable mesh. At 1cm2 measured by computed tomography, corroborating intraoperative [6]. Persons BL used resorbable perforated plates (25 x 25 x 0.6 mm) through a 1 cm2 antral access to the maxillary sinus and infraorbital floor in five patients without reporting complications. Serhan Tuncer showed 17 patients with an orbital floor fracture from 2002-2004, reconstructed with a resorbable plate by cutting it with scissors, curving it anatomically and adjusted to the orbital floor defect 0.5 mm posterior to the inferior orbital border, unreported skin or conjunctival closure complications [7-9].
Orbital fractures are common, sometimes difficult to manage, more frequent in men in the 2nd decade of life, accounting for up to 40% of craniofacial injuries [10]. Its management can be conservative (observational) or surgical considering: position of the eyeball, visual compromise, age of the patient, size / trace of the fracture, etc. The diagnosis is clinical-tomographic; the eye examination consists of eight aspects: vision, eye pressure, eye motility, pupillary examination, visual field, slit lamp eye examination, retinal examination and external examination. Some of these (vision, mobility and visual field) require a conscious and cooperative patient, however not all are absolute. The clinical data of an orbital fracture are: periocular edema, proptosis (in the acute stage), enophthalmos (advanced stage and large fracture), several authors associate it with a broad fracture of the floor of the orbit, ecchymosis, chemosis, V2 hypoesthesia and hemorrhage. Subconjunctival [11-13].In any rupture or open eye trauma, evaluate the general vision (with the patient conscious), eye protection, immediate ophthalmological management. The following signs should be considered as risks of ocular trauma (mainly due to possible rupture of the eyeball): 360° of subconjunctival hemorrhage, deformed pupil (beak, corectopia) and flat anterior chamber.
If the eyeball is intact, the eye pressure should be checked. If it is elevated by an orbital compartment syndrome (orbital swelling and retrobulbar hemorrhage) it can lead to optic neuropathy and blindness. This occurs in 3% of isolated orbital fractures [14]. In these cases, perform canthotomy and cantholysis immediately. Pressures less than 40 mmHg can be treated with drops to reduce eye pressure, but if conservative therapy fails, consider a canthotomy and cantolysis. A slit lamp examination can be performed, thoroughly evaluating the cornea and retina, detecting associated lesions (corneal abrasions, lens dislocations, hyphema, commotio retinae and retinal detachments). Commotio retinae is a common eye injury in these fractures (22%), followed by hyphema and corneal injuries. It is important to evaluate extraocular movement, mainly in children due to the so-called white eye syndrome, ("normal" eye but with limitation of extraocular movement). Green stem fractures are more common in children, causing cheating and muscle clamping, causing pain in eye movements, nausea, vomiting, and bradycardia that can simulate symptoms of a closed head injury.
The gold standard for imaging is Computed Tomography, as mentioned by Holmgren, finding tomographic ally that 12% of craniofacial injuries presented at least one maxillofacial fracture, being more frequent in orbit [15]. It is important that the patient avoid blowing his nose, since the air from the Sino nasal tract can be forced into the orbit and cause compartment syndrome, which can complicate causing blindness. Periorbital edema decreases with cold compresses. To ensure that the eyelids can be closed to protect the ocular surface (exposure of the eyeball), ophthalmic ointment or temporary tarsorrhaphy can be used. Some studies suggest antibiotic use, but there is little literature evaluating its specific action in isolated orbit fractures [16-18]. Mundinger fails to report convincing prophylactic evidence for antibiotic in medial wall and ceiling fractures [19]. However, intraoperative antibiotic administration is reported as a fundamental part of the management of orbital floor fractures, mainly [20].Those patients with pre-existing paranasal pathology may have an increased risk of developing orbital cellulitis, so it is necessary to prescribe antimicrobial [21].
Surgical management of orbital floor fractures begins by verifying ocular motility (forced induction tests). The incision and dissection must be careful, reach the orbital rim, dissect the sub periosteal plane towards the orbital floor, and then the entire surface involved cephalad (at 20°). In the deepest part of the orbital floor use a malleable retractor / retractor to lift the orbital tissues without hurting, improving visibility and identifying the fracture. Herniated orbital tissue can be found and must be treated delicately, avoiding unintentional penetration of the same when dissecting or avoiding projecting it to the fracture line, complicating the retraction of orbital fat, obstructing surgical visibility. Bone segments of the fracture that limit soft tissue elevation can be removed to improve orbital tissue mobility, identify the infraorbital nerve and mobilize adjacent tissue, separate segments of the orbital floor and mucosa of the maxillary sinus. Identify the extent of the fracture and the stable tissue (mainly posterior border) to place the implant; this is shaped and placed taking care that the size does not exceed dimensions, affecting the mobility and position of the eyeball. In severe fractures (eyeball compromise, significant loss of bone tissue, large extent of the fracture line (s), the posterior part of the orbital floor may be unstable or unidentifiable, making it difficult to place the implant, increasing the risk of ophthalmologic functional deficits. In these cases, it is suggested to use more rigid implants and fix them to the infraorbital or cantilever support edge towards the edge of the posterior orbital fracture. If the implant is projected too high, it can cause hyper Globus and ocular motility problems and if it is placed too deep, it can impact the optic nerve at the apex and cause loss of vision.
OBJECTIVES
To describe and analyze the clinical-epidemiological characteristics of orbital floor fractures treated with titanium mesh reconstruction for 5 years during the period from January 2013 to December 2018. Report the number of cases with orbital floor fractures. surgically treated and the association of orbital floor fractures with other fractures adjacent to the orbital cavity in patients treated surgically by the Maxillofacial Surgery service, Specialty Hospital “Dr. Bernardo Sepulveda Gutiérrez” National Medical Center Century XXI, IMSS. from January 2013 to December 2018.
MATERIAL AND METHODS
An observational, retrospective, descriptive research study was carried out for 5 years on the “clinical-epidemiological characteristics of orbital floor fractures, treated with titanium mesh reconstruction, in Maxillofacial Surgery service, Specialty Hospital “Dr. Bernardo Sepulveda Gutiérrez” National Medical Center Century XXI, IMSS, in 2013 -2018”. The inclusion criteria were: patients treated surgically with titanium mesh reconstruction of orbital floor fractures, adults, with computed tomography and clinical data on orbital floor fractures, any gender regardless of personal pathological history. Exclusion criteria: patients treated in other medical units or services, with no diagnosis of orbital floor fracture, minors, conservative management, or previous post-surgical sequelae. Information from clinical records was collected and noted on a checklist. Statistical analysis performed in SPSS-24. The results were reported in frequencies, means, percentages, and for parametric and median variables, interquartile ranges for non-parametric tests.
RESULTS
A total of 159 patients with some orbital floor fracture (Figure 1b) were presented to the Maxillofacial Surgery Service of CMN S. XXI, of whom 159 underwent surgery: 157 with reconstruction (titanium mesh) and 2 surgical explorations without implants. The mean age was: 39.35 years (max: 86 min: 18), the male gender being predominant: 84.27%, 70 patients presented only with an orbital floor fracture, 69 a medial wall and floor fracture, 20 an orbital floor fracture with another facial fracture, and 1% in panfacial fractures (Table 1). 84% were secondary to physical assault and 16% accidents of which 11% were by motorcycle, bicycle or falls and 5% by vehicle (Table 2); 97% presented periorbital edema, 40% with limited eye movements, 30% ecchymosis, 29% hyposphagma (Figure 2a-2d,Figure 3a-3c), 18% emphysema (Figure 1a), 88% diplopia, 1.25% presented amaurosis, 3 patients were treated in conjunction with ophthalmology: 1 had temporary tarsorrhaphy and 2 were treated for compartment syndrome (Table 1). The surgical approaches (Figure 4a-4b) used were: 90% subciliary and 10% transconjunctival. 9 patients with complications were reported: 3 with persistent diplopia, one due to transient postoperative edema, and two correcting with ophthalmological management (prime lenses) .The mesh was well adapted in these; 2 required a new mesh, in 3 there was a poor adaptation of the implant, correcting with repositioning, and 1 required surgical exploration without complications (Table 3).
|
Orbital Floor fractures |
Single Orbit Floor |
Orbit Floor + Medial Wall |
Floor of orbit and that they presented more than 2 associated fractures (including panfacial) |
||||||
|
|
|
Total |
D* |
I" |
CCO1 |
Nasal2 |
Mand/DA3 |
NOE 4 |
Panfacial5 |
|
Males:134 |
54 |
63 |
30 |
33 |
9 |
6 |
2 |
5 |
2 |
|
Females:25 |
16 |
6 |
6 |
0 |
2 |
1 |
1 |
0 |
0 |
|
|
Total: 69 |
36 |
33 |
20 |
11 |
7 |
3 |
5 |
2 |
|
Diseases |
Diabetes |
Arterial hypertension |
Other comorbidities |
|
|||||
|
Males |
10 |
2 |
03 male patients(1 HIV, 1 liver cirrhosos, 1 CKD**) |
|
|||||
|
Females |
1 |
5 |
02 female patients: 1 Rheumatoid Arthritis, 1 Osteopenia |
|
|||||
|
Total=23 |
11 |
7 |
|
||||||
|
signs and symptoms |
periorbite edema |
Diplopia |
Ecchymosis |
Emphysema |
Hyposphagma |
L.E.M |
C.Sx. |
Amaurosis |
|
|
Number of patients |
154 |
140 |
48 |
29 |
18 |
25 |
2 |
1 |
|
|
D*= right side I"= left side |
|
||||||||
|
CCO2= Orbito-zygomatic complex fracture |
|
||||||||
|
Nasal 2= nasal Fracture |
|
||||||||
|
Mand/DA2=Mandibular and/or dentoalveolar fracture |
|
||||||||
|
NOE4=Orbito-Naso-Ethmoidal |
|
||||||||
|
Painful fracture 2= All thouse fractures involve one or more fractures in each of the facial thirds |
|
||||||||
|
CKD**= Chronic Kidney Disease |
|
||||||||
|
L.E.M= Limitation of eye movements |
|
||||||||
|
C.Sx.= Compartment Syndorme |
|
|
|
|
|
|
|
|
|
Table 1: Characteristics of patients with orbital floor fractures
|
Gender |
Physical Aggression |
Accidents |
|
|
|
|
|
|
Motor Cycle |
Vehicular |
Bicycle |
Falls |
|
Males: 134 |
117 |
10 |
5 |
0 |
2 |
|
Females: 25 |
17 |
0 |
2 |
1 |
5 |
|
|
|
10 |
7 |
1 |
7 |
|
Total: 159 |
134 |
25 in accidents |
|
|
|
Table 2: Etiology of Orbital Floor Fracture
|
Orbital Floor Fractures |
Only Orbital Floor |
Orbital Floor + Mrdial Wall |
Orbital Floor+ 2 associated fractures(including panfacials) |
Total |
|
Males |
54 |
63 |
17 |
134 |
|
Females |
16 |
6 |
3 |
25 |
|
Total |
70 |
69 |
20 |
159 |
|
|
68 |
69 |
20 |
157 |
|
Titanium(Ti) mesh reconstruction |
|
|
|
|
|
|
1 Implant Scan 2 placing new mesh |
|
||
|
|
1 with double mesh |
|
||
|
|
2 re-interventions |
|
||
|
|
3 reposting same mesh |
|
|
|
|
Other Treatment |
2 Scans without mesh |
RAFI* of other facial fractures+ reduction of nasal fracture |
RAFI* of other facial fractues + reduction of nasal fracture |
|
|
Surgical Approach: 141 with a subciliary approach and 16 with a transconjunctival approach |
|
|
|
|
|
Complications |
persistant diploma: 05 In all the mesh was well placed |
new mesh placement |
Bad mesh adaptation |
surgical examination |
|
Total: 09 |
3 for transient edema 2 Management by Opthamology |
2 |
03 Corrected with repositioning |
01 without complication |
|
*RAFI= Anatomic reduction and internal fixation, Carried out with osteosynthesis material, based on AO facial Fracture Reduction Principals |
|
|
|
|
Table 3: Frequency of orbital floor fractures according to gender and treatment
 Figure 1a and Figure 1b: Coronal section computed tomography showing a fracture of the floor of the orbit with a marked medial wall involvement (red arrows) and the presence of subcutaneous emphysema (Yellow arrow)
Figure 1a and Figure 1b: Coronal section computed tomography showing a fracture of the floor of the orbit with a marked medial wall involvement (red arrows) and the presence of subcutaneous emphysema (Yellow arrow)
 Figure 2a-2d: Clinical Photographs with different degrees of edema and ecchymosis in patients with an orbital floor fracture
Figure 2a-2d: Clinical Photographs with different degrees of edema and ecchymosis in patients with an orbital floor fracture

Figure 3a-3c: Clinical Photographs with different degrees of hyposphagma and ecchymosis in patients with an orbital floor fracture
 Figure 4a: A Subciliary approach and placement of titanium mesh are observed in a right orbital floor fracture.
Figure 4a: A Subciliary approach and placement of titanium mesh are observed in a right orbital floor fracture.
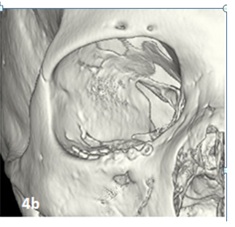 Figure 4b: Representative image of control CT (postoperative) od the same patient in figure 4a, postoperative for reconstruction with titanium mesh due to orbital floor fracture, where adequate coloration and attachment of the mesh is observed.
Figure 4b: Representative image of control CT (postoperative) od the same patient in figure 4a, postoperative for reconstruction with titanium mesh due to orbital floor fracture, where adequate coloration and attachment of the mesh is observed.
DISCUSSION
This research work was found to coincide with that who reported that of 78 patients with maxillofacial trauma, 66% were men with an age range between 15 and 35 years, who report the mean of 33 years, having in their study an age range of 17-87 years. It was shown that regardless of the approach used, good results were obtained in this study. The most common approach in this study was subciliary. A study [23].It mentions that in Mexico the institutions with the highest number of cases treated for eye trauma are the IMSS (Mexican Institute of Social Security) and the ISSSTE (Institute of Security and Social Services of State Workers), therefore confirms that the present study is carried out in one of the Institutions in Mexico with the highest influx of patients (IMSS). There are few studies in Latin America and Mexico with epidemiological and statistical data in relation to the number of cases that present an orbit fracture or in the case of this study of Orbital Floor Fracture, therefore, the estimated number of them is not available; however a study [24] globally globally, analyzing the latest publications mention that the geographical distribution of prevalent cases was similar to incident cases in 2017, having a higher prevalence by age of facial fractures in Central Europe with 68 cases per 100,000, likewise It mentions that Latin America and Western Europe have different age patterns, since in European countries they appear in groups over 70 years old, while in Latinos it is reported in young people. Which coincides with the sample given that the average age was 39.35 years (max: 86 min: 18), In the article [25] mention that for the World Health Organization (WHO) in 2020 Cranioencephalic Trauma is considered a transcendental public health problem because of the significant damage it causes to patients who suffer it; As we mentioned at the beginning of our study, it is for this reason that we consider it relevant to continue studies related to the incidence and prevalence of patients with orbital fractures (floor, medial wall, or other of the walls that make up the orbital vault), since in Mexico and Latin America there are few studies or follow-ups of the same.
CONCLUSION
Orbital fractures should be treated with measure; the importance of orbital floor fractures is related to the support of the eyeball and structures contained in the orbital cavity, and its proximity to the foramen and infraorbital nerve. Complications are related to improper implant placement. With this study it was found that the least traumatic surgery and precise anatomical reconstruction, together with the appropriate material for orbital reconstruction, will allow for speedy recovery and functionality. Currently there are different techniques to reconstruct the orbital floor. However, open surgery techniques are used more compared to endoscopy, possibly due to the difficult acquisition of the equipment or few studies on it. Large and complex fractures probably require specific patient-designed implants (PSI). If a patient with an orbital fracture is not treated in a timely manner, it may have complications such as compartment syndrome, optic neuropathy and / or blindness.
THANKS
We thank Dr. Daniel Juárez Rebollar, General Doctor and Resident of Neurosurgery, for his participation and help as a methodological advisor in this study.
CONFLICT OF INTEREST
Neither the authors nor any member has a financial or interest relationship (currently or in the last 12 months) with any entity producing, marketing, reselling or distributing health care products or services consumed by, or used in, the patients.
FINANCING
We have not received funding to carry out this study.
REFERENCES
- Marcelo RJ, Fernanda GVM, Jonathan R, Arocena MA, Medina AJ, et al. (2013) Classification and epidemiology of orbital fractures diagnosed by computed tomography. Argent.Radiol 77: 139-146.
- Rodriguez Perales MA, Pou Lopez VC, Villagra Siles E (2004) Orbital fractures managed at the Otorhinolaryngology and Head and Neck Surgery Service of the Central Military Hospital.Five year experience. An Orl Mex 48: 8-15.
- Bord SP, Linden J (2008) Trauma to the globe and orbit. Emerg Med Clin North Am 26: 97-103.
- Edward Chang W, Manolidis S (2005) Orbital Floor Fracture Management, Facial Plastic Surgery 21: 1-3.
- Ng P, Chu C, Young N, Soo M (1996) Imaging of orbital floor fractures. Australas Radiol 40: 264–268.
- Larry H, Hollier MD, Nicole Rogers BS, Edward Berzin MD, Samuel Stal MD, et al. (2015) Resorbable Mesh in the Treatment of Orbital Floor Fractures. J Craniofac Surg 14: 19-22.
- Persons BL, Wong GB (2002) Transantral endoscopic orbital floor repair using resorbable plate. J Craniofac Surg 13:483-488.
- Tuncer S, Yavuzer R, Kandal S, Demir YH, Ozmen S, et al. (2015) Reconstruction of Traumatic Orbital Floor Fractures With Resorbable Mesh Plate. J Craniofac Surg 18: 598-605.
- Jose RJ (2012) Anatomy of the eyeball and the orbit. Elsevier 1: 1-9.
- Boyette Jennings R, Pemberton John D, Juliana BV (2015) Management of orbital fractures: challenges and solutions. Clin Ophthalmol 9: 2127–2137.
- Cruz AA, Eichenberger GC (2004) Epidemiology and management of orbital fractures. Curr Opin Ophthalmol 15: 416–421.
- Hwang K, You SH, Sohn IA (2014) Analysis of orbital bone fractures: a 12-year study of 391 patients. J Craniofacial Surg 20:1218–1223.
- He D, Blomquist PH, Ellis E (2007) Association between ocular injuries and internal orbital fractures. J Oral Maxillofac Surg 65: 713–720.
- Holmgren EP, Dierks EJ, Homer LD, Potter BE (2004) Facial computed tomography use in trauma patients who require a head computed tomogram. J Oral Maxillofac Surg 62: 913–918.
- Andreasen JO, Jensen SS, Schwartz O, Hillerup Y (2006) A systematic review of prophylactic antibiotics in the surgical treatment of maxillofacial fractures. J Oral Maxillofac Surg 64: 1664–1668.
- Knepil GJ, Loukota RA (2010) Outcomes of prophylactic antibiotics following surgery for zygomatic bone fractures. J Craniomaxillofac Surg 38: 131–133.
- Zix J, Schaller B, Iizuka T, Lieger O (2013) The role of postoperative prophylactic antibiotics in the treatment of facial fractures: a randomised, double-blind, placebo-controlled pilot clinical study. Part 1: orbital fractures in 62 patients. Br J Oral Maxillofac Surg 51: 332–336.
- Mundinger GS, Borsuk DE, Okhah Z (2015) Antibiotics and facial fractures: evidence-based recommendations compared with experience-based practice. Craniomaxillofac Trauma Reconstr 8: 64–78.
- Chole RA, Yee J (1987) Antibiotic prophylaxis for facial fractures. A prospective, randomized clinical trial. Arch Otolaryngol Head Neck Surg. 113: 1055-1057.
- Ben Simon GJ, Bush S, Selva D, McNab AA (2005) Orbital cellulitis: a rare complication after orbital blowout fracture. Ophthalmology 112: 2030-2034.
- Malagon HH, Gonzalez M, Ayala UF, García C, Vilchis LR, et al. (2015) Long-term experience with the use of preformed absorbable implants for the treatment of orbital fractures. Plastic surgery 25: 97-105.
- Tomich G, Baigorria P, Orlando N, Méjico M, Costamagna C, et al. (2011) Frequency and type of fractures in maxillofacial trauma. Evaluation with multislice tomography with multiplanar and three-dimensional reconstructions. Rev Argent Radiol 75: 305-317.
- Ferraez P, Jose Luis Y, Romulo PM (2019) Epidemiological characteristics of ocular trauma, classified according to the ocular trauma score. Rev Med UAS 9: 143-150.
- Lalloo R, Lydia L, Catherine B, Castle C, Dingels Z, et al. (2020) Epidemiology of facial fractures: incidence, prevalence and years lived with disability estimates from the Global Burden of Disease 2017 study. Inj Prev Pg no: 1–9.
- Abosadegh Maher M, Rahma Shaifulizan AB (2018) Epidemiology and incidence of traumatic head injury associated with maxillofacial fractures: A global perspective. JIOH 10: 63-70.
Citation: Giselle JRA, Arlen CO, Daniel JR (2020) Clinical and Epidemiological Characteristics of Orbital Floor Fractures, Rebuilt with Titanium Mesh. J Transl Sci Res 3: 011.
Copyright: © 2020 Giselle JRA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

